Healthcare Payor Solutions
Automating Claims, Enhancing Member Experience & Enabling AI
Empowering payors with smarter workflows, seamless engagement, and AI‑enabled insights that improve performance.
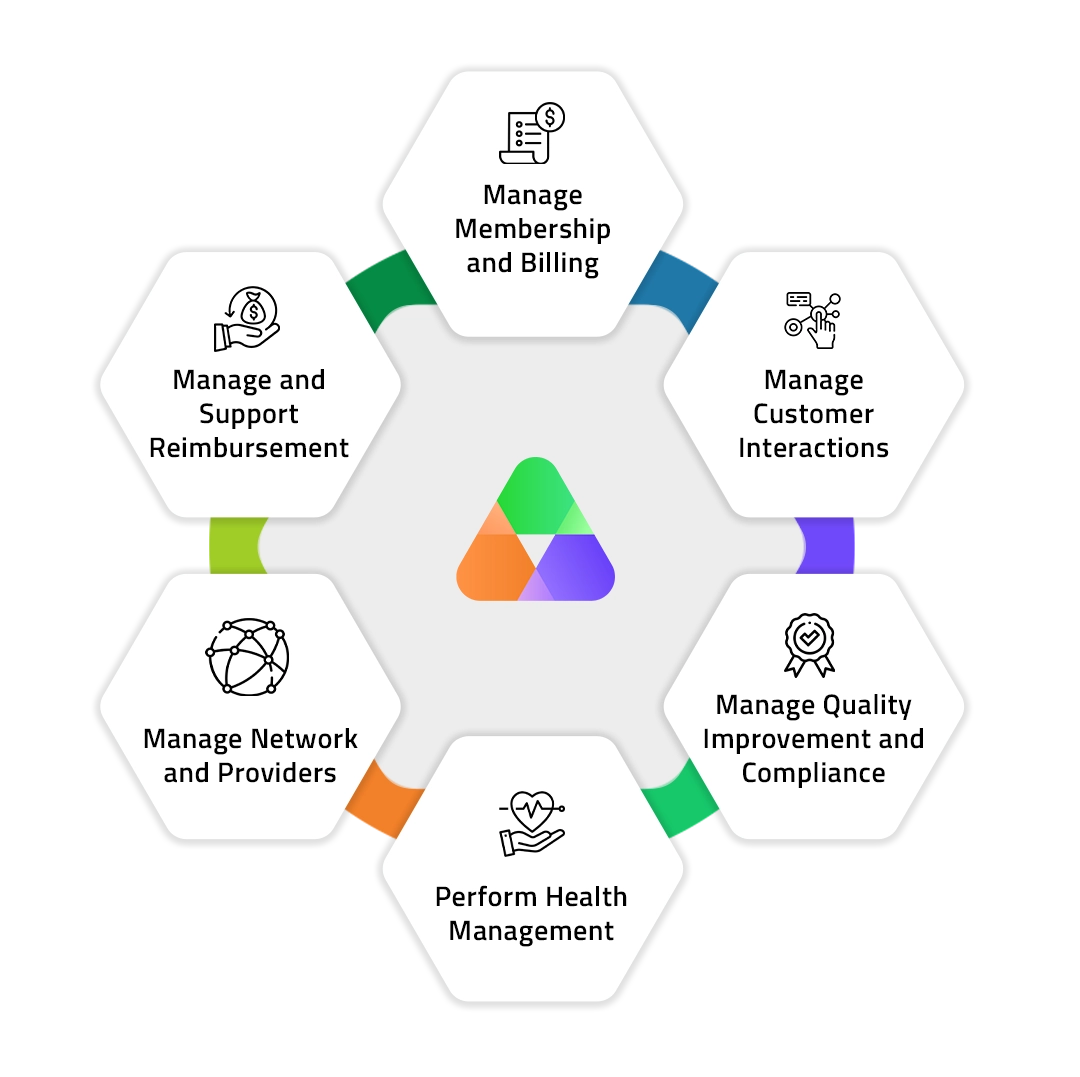

Deploy intelligent solutions that engage members effectively across every channel — increasing loyalty, improving retention, and strengthening brand trust.Deploy intelligent solutions that engage members effectively across every channel — increasing loyalty, improving retention, and strengthening brand trust.

Enable team collaboration and productivity by providing solutions that streamline communication, automate workflows, and improve access to information.

Unite data silos and apply advanced analytics and AI to reveal actionable insights to help make better, faster decisions on claims and operations.

Automating high‑volume claims workflows to reduce errors, shorten cycle times, and improve accuracy.
Build a world-class contact centre with self-service channels and support services for member enrolment, onboarding, inquiry handling, and proactive outreach.
Tools that simplify provider onboarding, credentialing, contracting, and directory management.
Automate audits across enrolment, claims adjudication, self-service channels, manual inquiries, and first-call resolution to reduce risk and ensure regulatory compliance.
Streamlining UM/PA workflows with intelligent routing, automation, and decision support.
Connecting core admin systems, provider data, claims data, and third‑party platforms for a unified view.
According to a leading industry report, healthcare payors can unlock up to $7 billion in operating income by optimising claims processing, membership management, customer interactions, and provider data management.
Watch Now
This case study highlights how a leading member-owned health insurer transformed its prior-authorization operations by replacing costly, manual fax processing with nVizion’s Intelligent Document Processing platform. By automating the ingestion, validation, and routing of millions of documents, the organization significantly reduced costs, improved turnaround times, and scaled operations—while freeing staff to focus on higher-value, member-centric work.
Download NowAccording to a leading industry report, healthcare payors can unlock up to $7 billion in operating income by optimising claims processing, membership management, customer interactions, and provider data management.
Watch Now
This case study highlights how a leading member-owned health insurer transformed its prior-authorization operations by replacing costly, manual fax processing with nVizion’s Intelligent Document Processing platform. By automating the ingestion, validation, and routing of millions of documents, the organization significantly reduced costs, improved turnaround times, and scaled operations—while freeing staff to focus on higher-value, member-centric work.
Download Now